STATISTICS AT A GLANCE
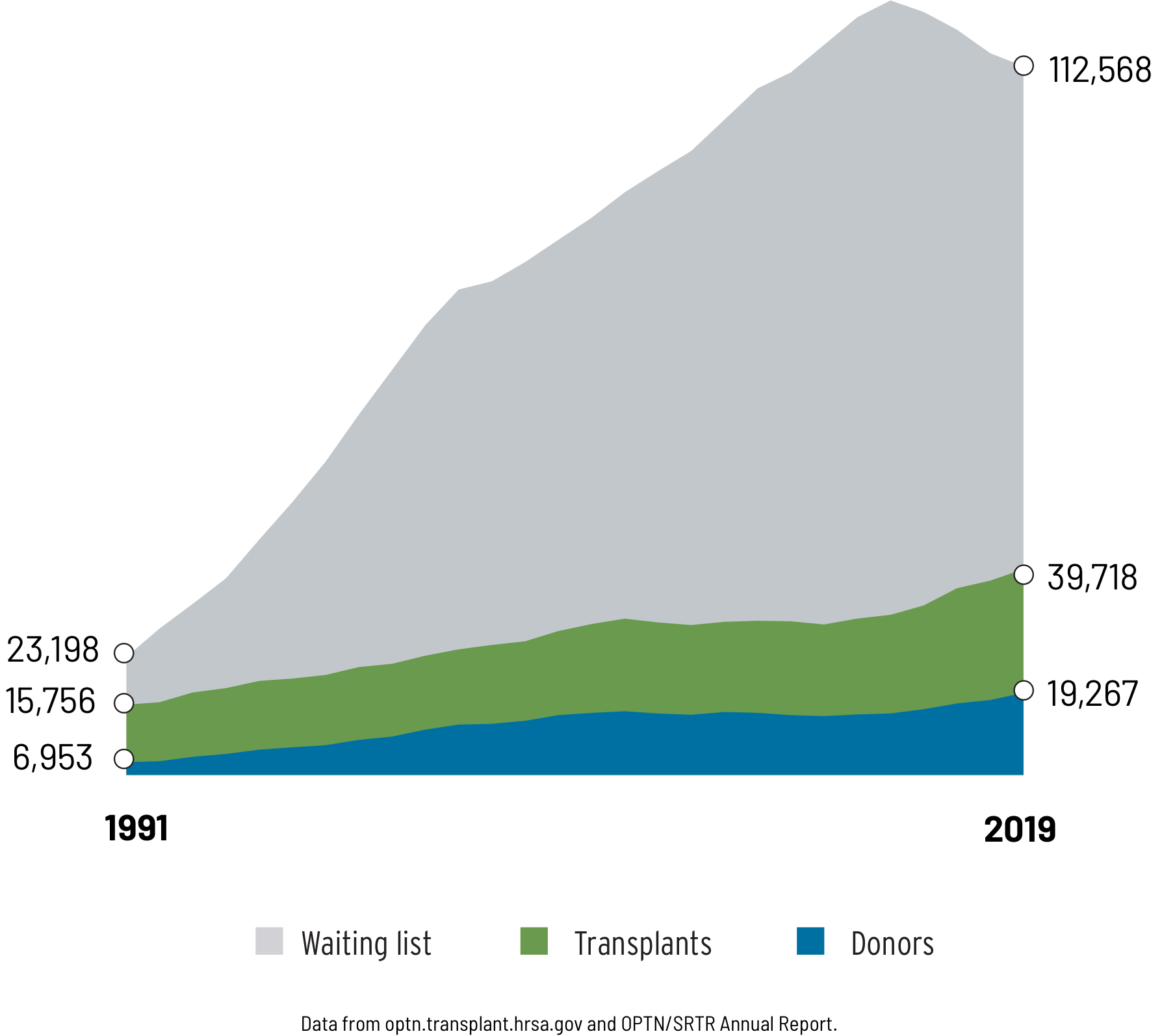
Historically, the number of people on the transplant waiting list continues to be much larger than the number of donors. Though this number is rising, many donor organs are still not used because they are considered unacceptable.
LUNGS VS. OTHER TRANSPLANTED ORGANS
ONLY 20%
OF AVAILABLE DONOR LUNGS ARE USED FOR TRANSPLANTATION*
*Each year this percentage is increasing due to technological
advancements
80%
ARE NOT USED
Yet, it is estimated that 40% of these lungs are still usable.
BY COMPARISON:
-
70%-80%
of available donor kidneys are used for transplantation
-
75%
of available donor Livers are used for transplantation
-
30%
of available donor Hearts are used for transplantation
CHALLENGES IN TRANSPLANTATION
The current process that precedes the acceptance of a lung for transplant is complex. Due to logistical challenges and incomplete information, transplant surgeons are often forced to make time-critical decisions under conditions that are not ideal.
- LOGISTICAL CHALLENGES
- INADEQUATE INFORMATION
- LIMITED TIME
WHAT IS EVLP?
EVLP is a platform that transplant physicians can use to assess donor lungs outside of the donor body.
-
EVLP may allow for extended lung preservation.
-
Increased preservation time makes it possible for organs to be transported over greater distances, therefore allowing optimized scheduling of surgical procedures.
-
EVLP procedure allows for data collection and live video feeds that help with decision making.
NORMOTHERMIC ASSESSMENT
- Removes lungs from a less than optimal environment (brain death)
- Allows for reassessment of DCD lungs
- Allows for recruitment with no hemodynamic consequence
- Allows for serial vein sampling
- Obtains lung x-ray images without surrounding tissue interference
- Performs thorough bronchoscopies at regular intervals
- Captures/shares data not consistently collected during lung evaluation in ICU
- Late organ offer
- Primary center declines
- Donor time constraints
- Family wishes
- Recipient needs
- Travel
- Plasmapheresis
- Pre-transplant cross-match
- Change in recipient
- Laterality of lungs
- Operational limitations
- Procurement and transplant surgeon availability
HOW DOES EVLP DIFFER FROM STANDARD TRANSPLANTATION PRACTICES?
In the past, there was only one path to transplantation called static cold storage (SCS): taking lungs that were deemed suitable for transplant, flushing them with cold preservation solution, and transporting them to the transplant center within a limited time frame. Today, we are able to extend that time frame by taking lungs that would not be suitable for transplant, flushing them with cold preservation solution, and transporting them for EVLP to re-evaluate the lungs. After the transplant physician accepts the lungs while on EVLP, the lungs are cooled down again, flushed with cold preservation solution, and shipped to a transplant center on ice.
| SCS | EVLP | |
|---|---|---|
| Preservation Method | Static Cold Storage Cell activity is slowed down and requirements for oxygen and essential nutrients is reduced to prevent organ deterioration. |
Static Cold Storage Donor lungs are preserved with static cold storage method
from procurement to the beginning of EVLP, and from the end of EVLP to transplantation.
EVLP Under normal conditions lung cells and tissues remain viable for several hours. |
| Assessment Time |
LIMITED |
EXTENDED |
| Preservation Time |
Maximum 4-6 HR |
Up to 16 HR |
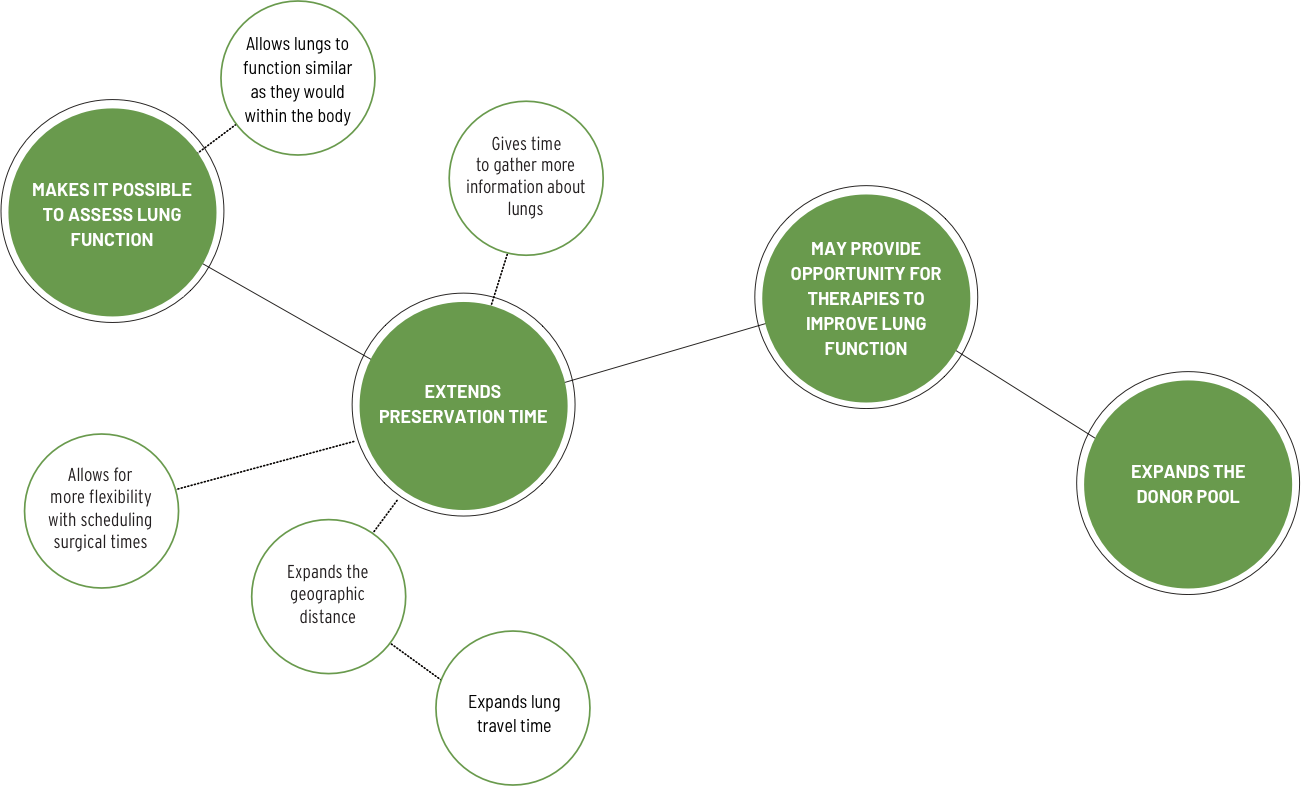
EVLP POTENTIAL
Discover the many benefits that EVLP can offer the field of lung transplantation:
DONOR LUNGS
| EXAMPLES OF NON-TRADITIONAL CASES | ||
|---|---|---|
| 01 |
Intraoperative Declines |
|
| 02 |
DCD |
|
| 03 |
Procurement of lungs by other qualified transplant center teams |
|
| 04 |
Utilization of procurement teams local to OPOs |
|
| 05 |
Back up of double lung perfusions with single lung recipients |
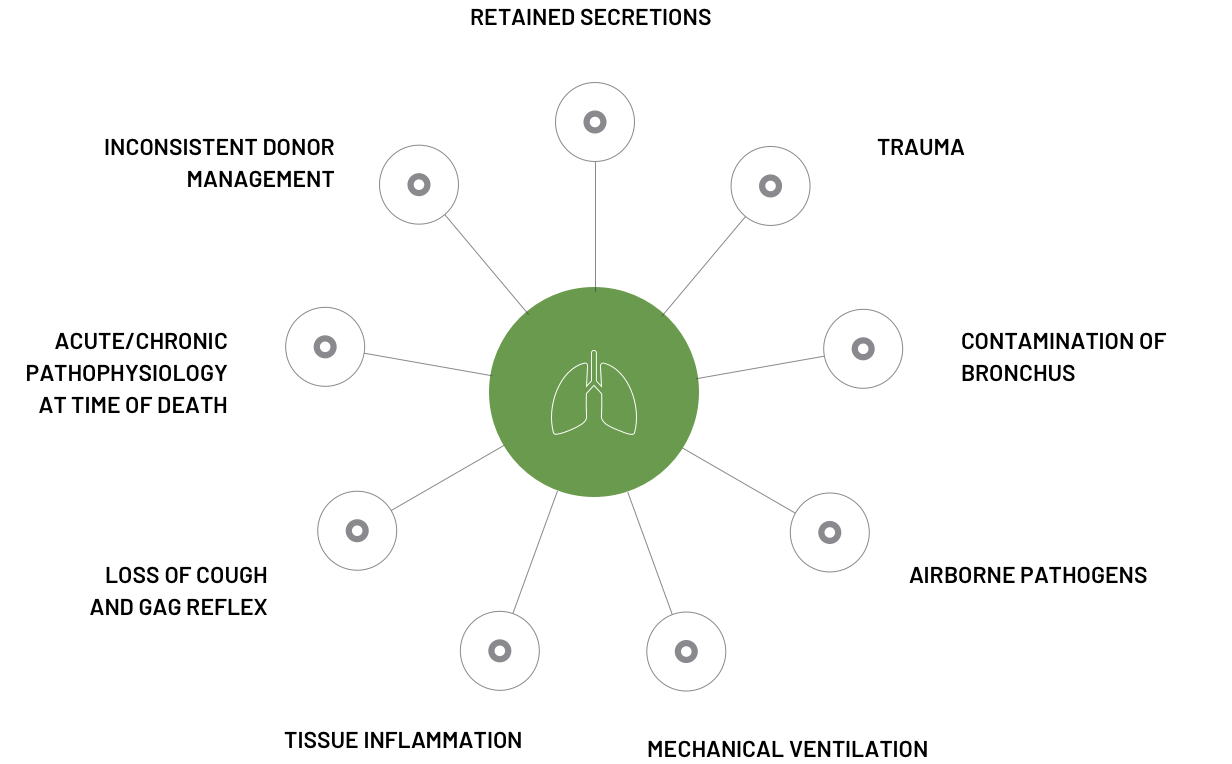
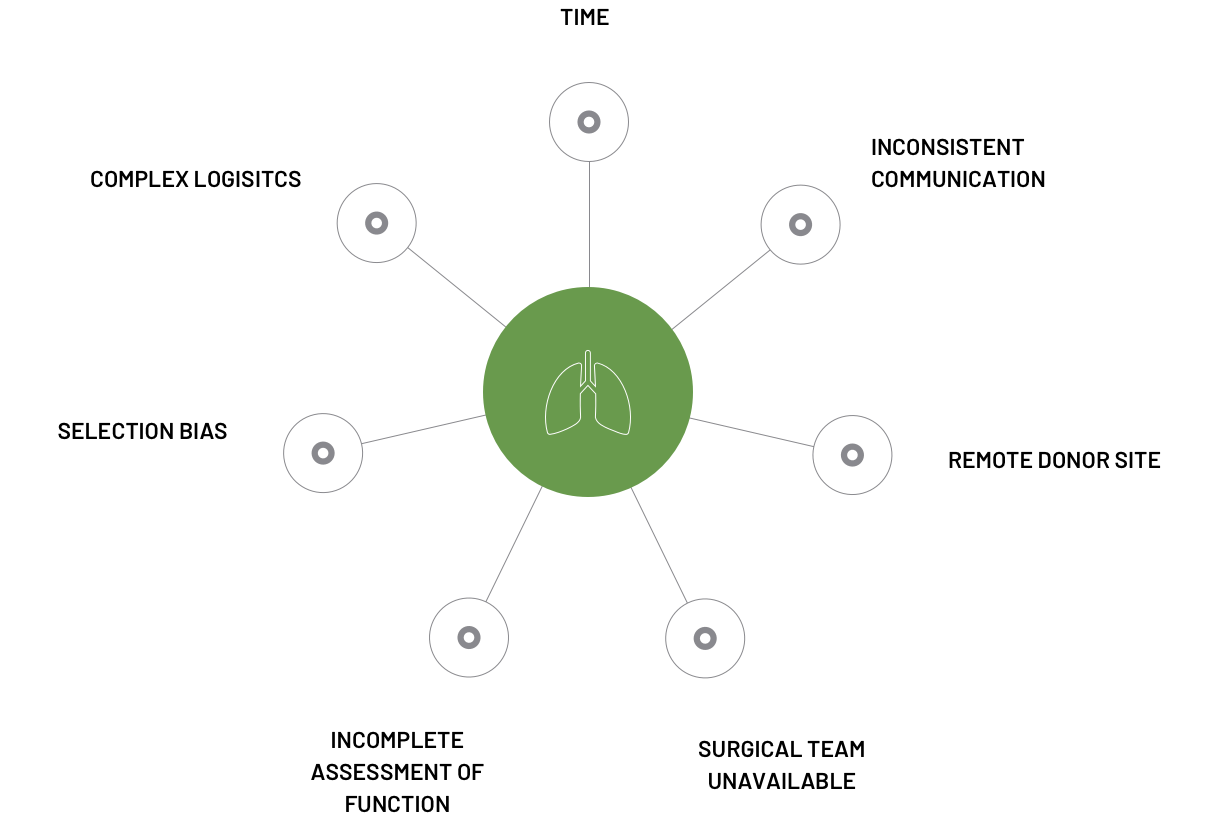
FACTORS COMPROMISING
EVLP TIMELINE
FIRST EVLP TRANSPLANT
In Sweden, ex-vivo lung perfusion is carried out for the first time on a human donor lung. The results of this procedure guide the first successful clinical lung transplantation from a non-heart-beating donor.

INITIALLY REJECTED LUNG
First transplant of a nonacceptable donor lung following EVLP.

TORONTO CLINICAL EXPERIENCE
Clinical trial concludes that transplantation of high-risk donor lungs that are physiologically stable during 4 hours of ex vivo perfusion lead to results similar to those obtained conventionally.

FIRST EVLP TRANSPLANT IN UNITED STATES
First lung transplantation with the application of remote EVLP, wherein the donor lungs are transported from the donor hospital to a center for EVLP and then transported to another hospital for transplantation into the recipient. It is also the first case of lung transplantation in the United States utilizing EVLP for functional optimization leading to successful transplantation.


FUTURE DIRECTION FOR EVLP1
-
NEAR-TERM
- Further optimization of EVLP
- EVLP used for semielective lung transplantation
- Adaptation for pediatric lung transplantation
-
MID-TERM
- EVLP performed in centralized hubs
- Decrease in costs
-
LONG-TERM
- EVLP used to rationally enhance donor lungs
EVLP IMPACT
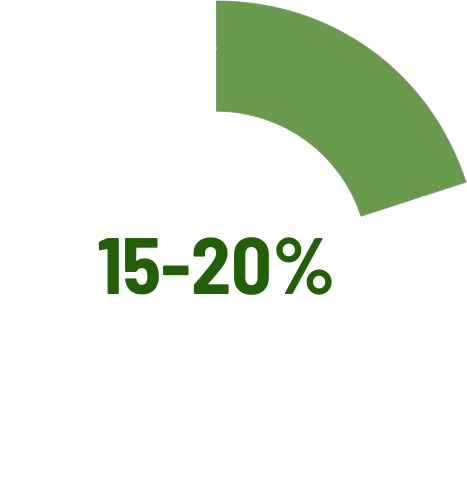
IMPACT OF EVLP ON ORGAN UTILIZATION
EVLP HAS INCREASED THE NUMBER OF TRANSPLANTABLE LUNGS BY 15-20% AT SOME TRANSPLANT CENTERS2
IMPACT OF EVLP ON PATIENT OUTCOMES3
Systematic review and meta-analysis was performed to evaluate the outcomes of EVLP conducted for marginal donor lungs.
PATIENTS
- 8 STUDIES
- 2 GROUPS
- 16% were patients with EVLP
84% were patients without EVLP
POST TRANSPLANT OUTCOMES WERE SIMILAR
Between EVLP-treated and Standard Lung Transplants
with respect to the length of postoperative intubation, postoperative extracorporeal life support/extracorporeal membrane oxygenation use, length of intensive care unit stay, length of hospital stay, 72-hour primary graft dysfunction of grade 3, 30-day survival, or 1-year survival (all P values > .05).
REFERENCES:
- Artificial Organs, Volume: 44, Issue: 1, Pages: 12-15, First published: 24 October 2019, DOI: (10.1111/aor.13571).
- Ex Vivo Lung Perfusion: A Key Tool for Translational Science in the Lungs. Tane S., Noda K., Shigemura N. (2017) Chest, 151 (6), pp. 1220-1228.
- Outcomes of marginal donors for lung transplantation after ex vivo lung perfusion: A systematic review and meta-analysis. Tian, Dong et al. The Journal of Thoracic and Cardiovascular Surgery, Volume 159, Issue 2, 720 - 730.e6






“ [With EVLP] we have been able to utilize some lungs that otherwise would not have been used for transplant.”
Dr. Matthew Hartwig Transplant Surgeon, Duke University